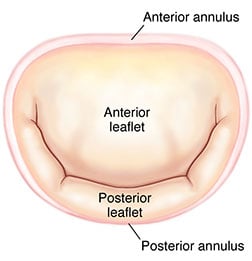
Mitral Annulus
The mitral valve is an atrio-ventricular valve, separating the left atrial chamber from the left ventricle. The mitral annulus constitutes the anatomical junction between the ventricle and the left atrium, and serves an insertion site for the leaflet tissue. It is often divided segmentally according to the site of leaflet insertion (the anterior or posterior annulus). The anterior portion of the mitral annulus is attached to the fibrous trigones and is generally more developed than the posterior annulus. The right fibrous trigone is a dense junctional area between the mitral, tricuspid, non-coronary cusp of the aortic annuli and the membranous septum. The left fibrous trigone is situated at the junction of both left fibrous borders of the aortic and the mitral valve. It was believed for many years that this portion of the annulus could not increase in circumference because of its relation to the trigones. Autopsy and 3-dimensional imaging studies have proven that this area, however, does in fact dilate in pathologic conditions which trigger mitral regurgitationHueb AC, Jatene FB, Moreira LF, Pomerantzeff PM, Kallas E, de Oliveira SA. Ventricular remodeling and mitral valve modifications in dilated cardiomyopathy: new insights from anatomic study. J Thorac Cardiovasc Surg 2002 December;124(6):1216-24.,Ahmad RM, Gillinov AM, McCarthy PM et al. Annular geometry and motion in human ischemic mitral regurgitation: novel assessment with three-dimensional echocardiography and computer reconstruction. Ann Thorac Surg 2004 December;78(6):2063-8.,Topilsky Y, Vatouri O, Watanabe N et al. Real-time 3-dimensional dynamics of functional mitral regurgitation: a prospective quantitative and mechanistic study. J Am Heart Assoc. 2013 May 31;2(3):e000039.
The mitral annulus is less well developed at the insertion site of the posterior leaflet. This segment is not attached to any fibrous structures, and the fibrous skeleton in this region is discontinuous. This posterior portion of the annulus is prone to increase its circumference in the setting of mitral regurgitation in association with left atrial or left ventricle dilation; correction of the annular dimension to normal is therefore an essential part of reconstructive degenerative mitral valve surgery. The mitral annulus is saddle shaped, and during systole the commissural areas move apically while annular contraction also narrows the circumference. Both processes aid in achieving leaflet coaptation, and may be affected by processes such as annular dilatation and calcification3. The mitral annulus is surrounded by several important anatomic structures which must be respected during mitral valve surgery, including the aortic valve, the coronary sinus, and the circumflex artery.
* Modified from Carpentier A, Adams DH, Filsoufi F. Carpentier’s Reconstructive Valve Surgery. From Valve Analysis to Valve Reconstruction. 2010 Saunders Elsevier.