Non-surgical Management
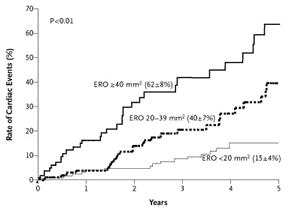
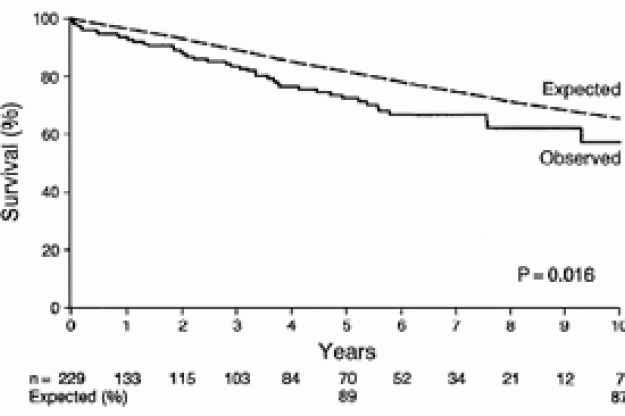
As current existing guidelines do not recommend surgery for asymptomatic or mildy symptomatic patients1 , there is a large cohort of patients with significant mitral regurgitation that do not undergo surgery, thus allowing for observational studies of outcomes in non-surgically treated cohorts. Additionally, before expanded application of mitral valve repair in the 1990s, cohorts of symptomatic patients with mitral valve prolapse were followed on medical therapy allowing determination of natural history of mitral regurgitation. Mitral valve prolapse with severe regurgitation reduces long-term survival irrespective of medical therapy. It appears that the prolapse itself is not the cause of mortality or morbidity (cardiac event rates are extremely low for the entire population with prolapse), but it is severe regurgitation and consequent left ventricular dilatation that results in morbidity2 ,3 . Heart failure, arrhythmia, endocarditis and stroke are the leading causes of death. Enriquez-Sarano and colleagues have performed analyses to define which group of patients with mitral regurgitation are at greatest risk of cardiac events4 , 5 , 6 . Notably, when considering asymptomatic patients, the greater the severity of mitral regurgitation (preferably determined by quantitative echocardiography), the higher the frequency of cardiac events irrespective of a normal ventricular function (Figure 1). Other risk factors for cardiovascular morbidity include atrial fibrillation, left atrial enlargement, age > 50 years and thickening of mitral leaflets7 – presence of these factors implies a reduced life expectancy if mitral regurgitation is uncorrected. Current evidence from surgical cohorts, suggests that mitral valve repair (assuming an operative mortality below 1%) yields a better outcome (survival and freedom from cardiac events) compared to the outcomes observed in non-surgically treated patients with severe regurgitation. For example mitral valve repair in patients with good ventricular function has a long term survival similar to expected survival in age matched cohorts 8 , 9 , whereas long term follow-up of patients with mitral valve prolapse treated medically shows a reduced survival compared to expected survival10 (Figure 2).
It should be emphasized that the alternative to surgical therapy is, strictly speaking, not medical therapy, but observation, as there are no pharmacological options for treatment of severe mitral regurgitation. Data supporting the role of any medical treatment – particularly vasodilators – in the management of severe regurgitation due to degenerative mitral valve disease is scant11 . Indeed it has been suggested that vasodilator therapy can lead to paradoxical worsening in mitral regurgitation by shifting the prolapse earlier in the cardiac cycle12 . Vasodilator therapy can also mask left ventricular dysfunction and result in (potentially deleterious) delay to mitral valve surgery. According to current guidelines, there is little role for pharmacological treatment in the management of severe mitral regurgitation1.
(*) Modified from Enriquez-Sarano M, Avierinos JF, Messika-Zeitoun D, et al: Quantitative determinants of the outcome of asymptomatic mitral regurgitation. New Engl J Med 352(9):875-83 2005. Copyright © 2005 Massachusetts Medical Society. All rights reserved.
(**) Modified from Ling LH, Enriquez-Sarano M.M, Long-term outcomes of patients with flail mitral valve leaflets. Coron Artery Dis. 2000 Feb;11(1):3-9. Review. Lippincott Williams & Wilkins
- 1Bonow RO, Carabello B, de Leon AC et al. ACC/AHA Guidelines for the Management of Patients With Valvular Heart Disease. Executive Summary. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients With Valvular Heart Disease). J Heart Valve Dis 1998 November;7(6):672-707.
- 2St John SM, Weyman AE. Mitral valve prolapse prevalence and complications: an ongoing dialogue. Circulation 2002 September 10;106(11):1305-7.
- 3Enriquez-Sarano M, Tajik AJ. Natural history of mitral regurgitation due to flail leaflets. Eur Heart J 1997 May;18(5):705-7.
- 4Zoghbi WA, Enriquez-Sarano M, Foster E et al. Recommendations for evaluation of the severity of native valvular regurgitation with two-dimensional and Doppler echocardiography. J Am Soc Echocardiogr 2003 July;16(7):777-802.
- 5Enriquez-Sarano M. Timing of mitral valve surgery. Heart 2002 January;87(1):79-85.
- 6Enriquez-Sarano M, Avierinos JF, Messika-Zeitoun D et al. Quantitative determinants of the outcome of asymptomatic mitral regurgitation. N Engl J Med 2005 March 3;352(9):875-83.
- 7Avierinos JF, Gersh BJ, Melton LJ, III et al. Natural history of asymptomatic mitral valve prolapse in the community. Circulation 2002 September 10;106(11):1355-61.
- 8Mohty D, Orszulak TA, Schaff HV, Avierinos JF, Tajik JA, Enriquez-Sarano M. Very long-term survival and durability of mitral valve repair for mitral valve prolapse. Circulation 2001 September 18;104(12 Suppl 1):I1-I7.
- 9Braunberger E, Deloche A, Berrebi A et al. Very long-term results (more than 20 years) of valve repair with carpentier's techniques in nonrheumatic mitral valve insufficiency. Circulation 2001 September 18;104(12 Suppl 1):I8-11.
- 10 Ling LH, Enriquez-Sarano M, Seward JB et al. Clinical outcome of mitral regurgitation due to flail leaflet. N Engl J Med 1996 November 7;335(19):1417-23.
- 11Hayek E, Gring CN, Griffin BP. Mitral valve prolapse. Lancet 2005 February 5;365(9458):507-18.
- 12Kizilbash AM, Willett DL, Brickner ME, Heinle SK, Grayburn PA. Effects of afterload reduction on vena contracta width in mitral regurgitation. J Am Coll Cardiol 1998 August;32(2):427-31.