Minimally Invasive Heart Surgery
We have helped pioneer small access incision valve surgery. We will always make the smallest possible incision for safe and efficient surgery. In general, incisions are normally closed with stitches beneath the skin that dissolve in 2-3 months, minimizing visual scar tissue.
Mitral valve repair is the gold standard procedure for patients who require surgery for mitral valve disease1. This is particularly important in the setting of degenerative disease where repair rates of close to 100% are achievable2. Today, many patients are candidates for less invasive mitral valve surgery. Minimally invasive surgery should ensure procedural safety and the ability of the surgeon to perform a durable mitral valve repair3.
Our less invasive approach is a limited, 7-8 cm, lower midline skin incision, using standard cardiopulmonary bypass techniques with central cannulation. This limited incision also provides sufficient exposure for tricuspid and aortic valve repair or replacement if needed.
Our limited skin incision sternotomy achieves all the goals of minimally invasive surgery:
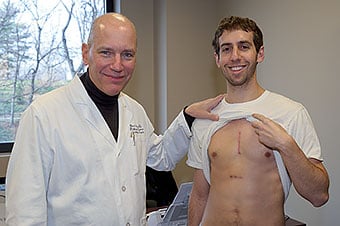
- Excellent cosmesis and very high patient satisfaction (the scars are smaller and less visible).
- Minimizing trauma with excellent post-operative pain control (most of our patients do not utilize narcotics after leaving the hospital).
- Low rates of bleeding and transfusion (our re-exploration rate for bleeding is <1%).
- The ability to perform any reconstructive technique that would be used in a standard sternotomy, with very high repair rates (our most recent series documented a repair rate exceeding 99% in an all-comers population of degenerative disease regardless of complexity).
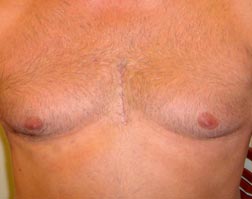
When fully healed the less invasive skin incision sternotomy scar is concealed by clothing, even when the patient wears low-necked clothing. In some women the scar is well concealed by their brassiere. For all these reasons, we feel the limited lower midline skin incision is the most flexible approach to the heart, and it is the approach we use in most patients.
Not all of our patients are suitable for minimally invasive surgery. Operating through small incisions is more technically challenging and in some cases could reduce the safety of the procedure. Patients who require additional cardiac procedures like coronary artery bypass surgery, elderly patients, patients with very diseased arteries, and patients with very weakly contracting hearts are generally, not suitable for this approach. Our paramount objective is safety first, and then to ensure an excellent valve repair, with no residual leakage, and minimal morbidity. Our surgeons perform repairs through small incisions whenever they believe they can achieve an excellent quality valve repair with a low risk to the patient (which is true for the majority of patients we see in our clinic today).
* Castillo JG, Milla F, Anyanwu AC, Adams DH. Video-atlas on minimally invasive mitral valve surgery-The David Adams technique. Ann Cardiothorac Surg 2013;2(6):828-832.
- 1David TE, Armstrong S, McCrindle BW, et al. Late outcomes of mitral valve repair for mitral regurgitation due to degenerative disease. Circulation 2013;127:1485-92. [PubMed]
- 2Castillo JG, Anyanwu AC, Fuster V, et al. A near 100% repair rate for mitral valve prolapse is achievable in a reference center: implications for future guidelines. J Thorac Cardiovasc Surg 2012;144:308-12. [PubMed]
- 3Suri RM, Vanoverschelde JL, Grigioni F, et al. Association between early surgical intervention vs watchful waiting and outcomes for mitral regurgitation due to flail mitral valve leaflets. JAMA 2013;310:609-16. [PubMed]